|
11 also found that 74% of silicotic patients had enlarged mediastinal lymph nodes and 66% of exposed workers had evidence of lymph node calcification. The classical features of patients with silicosis are diffuse interstitial shadowing with bilateral enlargement of hilar lymph nodes, which may or may not be calcified 10. Silicosis: Silicosis is caused by the inhalation of free silica particles during occupational exposure –such as in mining, drilling, and sandblasting –which leads to a fibrous tissue reaction in the lungs 9.Lymphoma: more common in Hodgkin lymphoma than non-Hodgkin lymphoma.Amorphous, punctate, or eggshell-like calcifications may also be seen and are suggestive of a chronic condition, occurring in 3% of patients after 5 years and in 20% after 10 years 8. In general, when multiple lymph node groups in the hila and mediastinum are symmetrically enlarged in a young patient, sarcoidosis is the most likely diagnosis. The left paratracheal nodes and the aortopulmonary window nodes are also commonly enlarged 7. 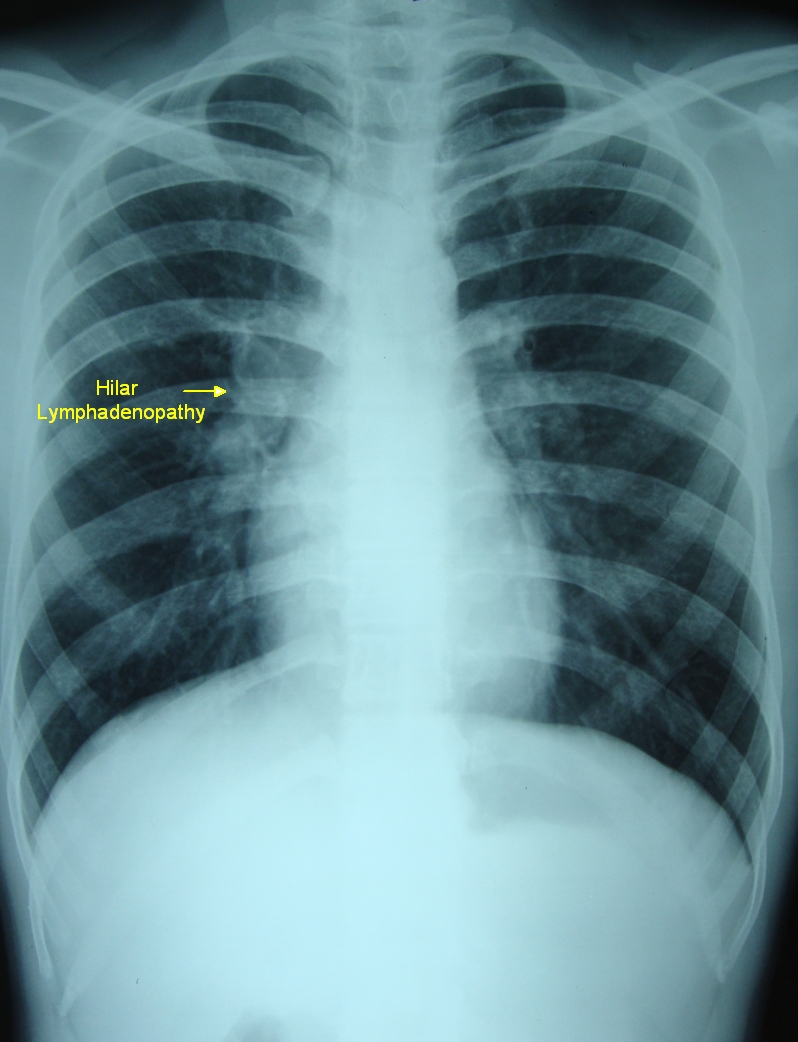
The most common pattern is bilateral hilar and right paratracheal lymphadenopathy, also known as Garland’s triad. Lymphadenopathy is seen in stages 1 and 2. Five radiological stages of intrathoracic changes have been defined: stage 0, no visible intrathoracic finding stage 1, lymphadenopathy only stage 2, lymphadenopathy with parenchymal infiltration stage 3, parenchymal disease only and stage 4, pulmonary fibrosis 6. Sarcoidosis: Sarcoidosis is a systemic granulomatous disease that affects primarily the lung and lymphatic system.Bilateral hilar lymphadenopathy causesīilateral hilar lymphadenopathy or bilateral hilar lymph node enlargement can arise from many causes, which include 1: Maximum greatest axial diameters show wider variation, ranging from 10 to 25 mm 5. Other authors use the following standard maximum normal short-axial diameters for nodal regions: region 7, 12 mm regions 4 and 10R, 10 mm and other regions, 8 mm. The generally accepted size criterion for mediastinal lymph node enlargement (>10 mm along the short axis) has been applied to all patients when staging lymphoma or bronchogenic carcinoma 4. The shortest axial diameter appears to be a more useful parameter than the greatest axial diameter, although a different threshold should be used for each nodal station 3. Commonly used metrics for lymph node measurement include the maximum and minimum axial diameters, and the ratio of these two values 2. Bilateral hilar lymphadenopathy is a radiographic term for the enlargement of mediastinal lymph nodes and is most commonly identified by a chest x-ray.įor the diagnosis of pathologically enlarged nodes, information about normal node size is required. The overall evaluation of lymphadenopathy, with a focus on findings suggestive of malignancy, as well as an approach to the patient with unexplained lymphadenopathy, will be reviewed.Bilateral hilar lymphadenopathy treatment Bilateral hilar lymphadenopathyīilateral hilar lymphadenopathy is a bilateral enlargement of the lymph nodes of pulmonary hila 1. While modern hematopathologic technologies have improved the diagnostic yields of fine-needle aspiration, excisional biopsy remains the initial diagnostic procedure of choice. Unexplained lymphadenopathy without signs or symptoms of serious disease or malignancy can be observed for one month, after which specific testing or biopsy should be performed. In addition, a complete exposure history, review of associated symptoms, and a thorough regional examination help determine whether lymphadenopathy is of benign or malignant origin. Knowledge of these risk factors is critical to determining the management of unexplained lymphadenopathy. Key risk factors for malignancy include older age, firm, fixed nodal character, duration of greater than two weeks, and supraclavicular location. The critical challenge for the primary care physician is to identify which cases are secondary to malignancies or other serious conditions. Among primary care patients presenting with lymphadenopathy, the prevalence of malignancy has been estimated to be as low as 1.1 percent. The majority of patients presenting with peripheral lymphadenopathy have easily identifiable causes that are benign or self-limited.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
